Injuring your back or spine while at work or due to a workplace accident can be debilitating. WorkSafe Queensland provides coverage for chiropractic treatment services to help affected workers access the health care for rehabilitation without the financial burden.
This guide includes the eligibility criteria, application process, and chiropractic treatment covered for WorkCover claims.
What Chiropractic Services are Covered by WorkCover?
Chiropractors are listed as approved registered providers for WorkCover claims. The specific Chiropractic services covered can be found in the Table of Costs guide for Chiropractic services (effective 1 August 2025).
Consultations
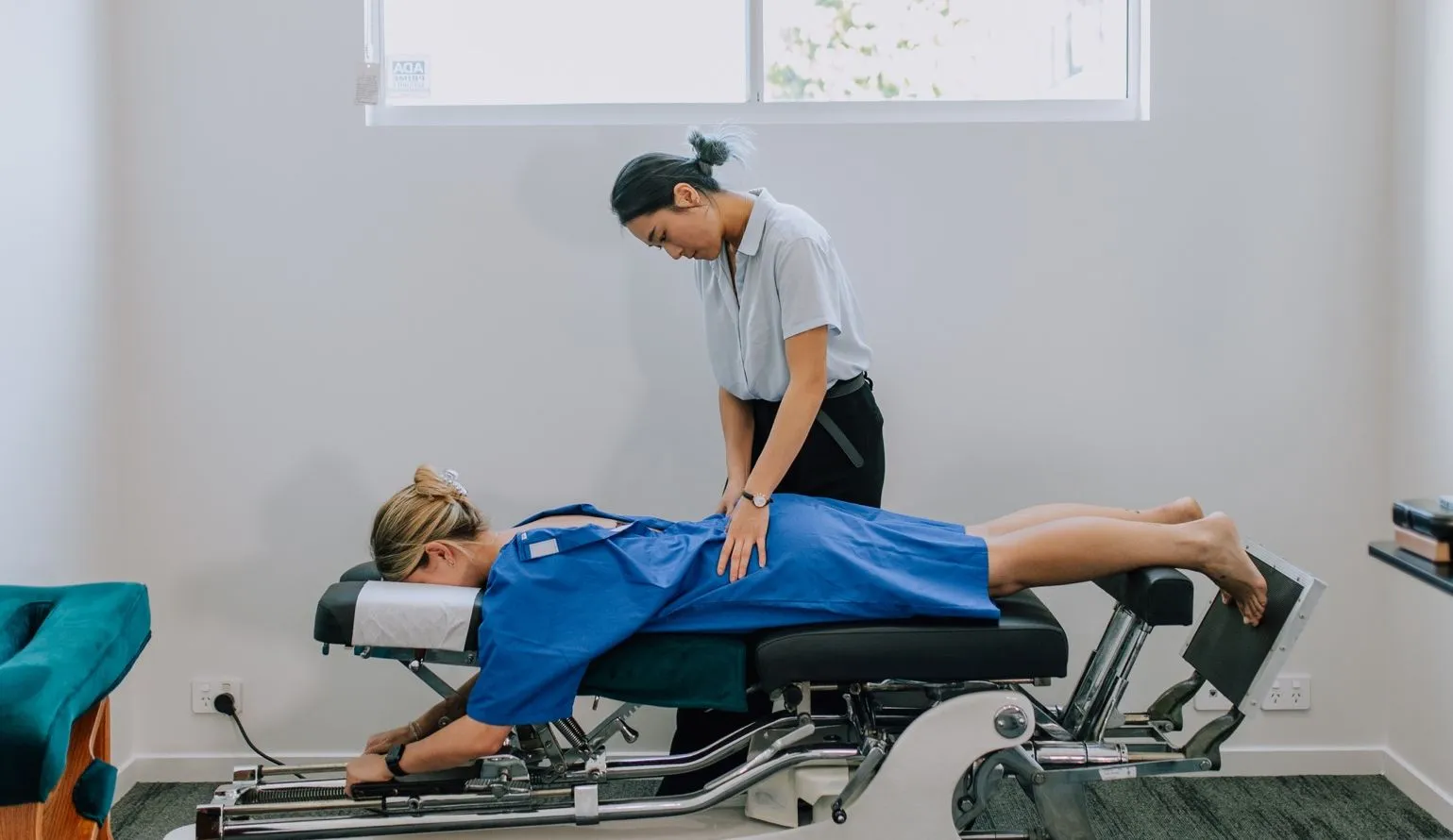
Consultation services with a chiropractor include physical assessments to identify the nature of the injury, treatment application, goal setting, creating a treatment plan, and communication with the insurer on the recovery plan.
Initial consultations are fully covered and do not require insurer pre-approval. In the initial consultation, your chiropractor will conduct a physical assessment to identify the nature of the injury, create a treatment plan based on your recovery goals, and apply treatments like manual adjustments.
The first five subsequent consultations are automatically covered. Coverage for the cost of additional consultations will require approval of a Provider Management Plan (PMP), which is prepared by the chiropractor.
WorkCover also does not cover multiple initial or subsequent consultations for the same injured individuals on the same day. This means that if you book two chiropractic appointments on the same day, only the first appointment will be covered.
X-Ray Imaging
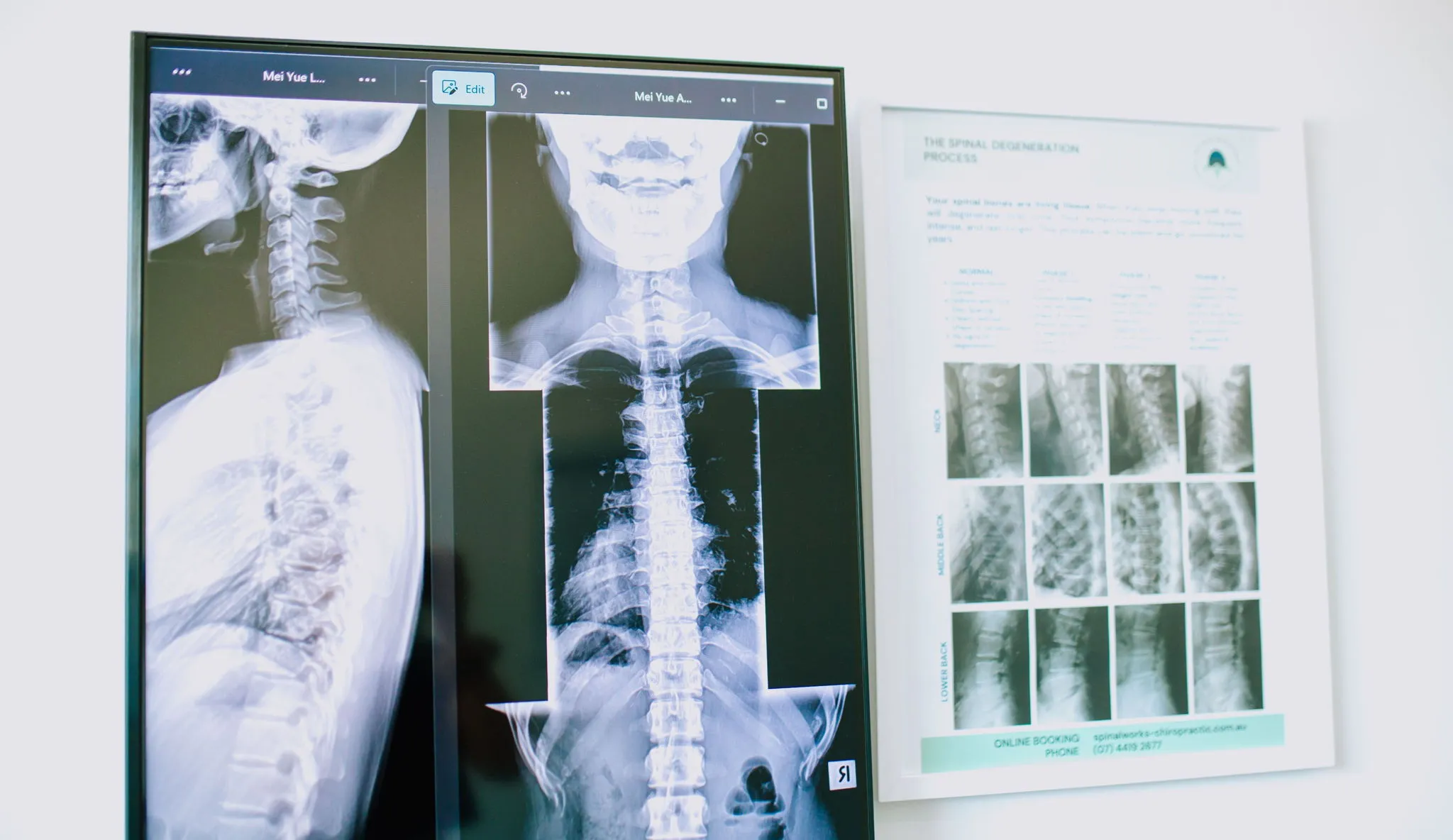
The cost of X-Ray imaging is covered when required for chiropractic diagnosis. Scans include X-Rays of the spine’s cervical, thoracic, and lumbosacral areas. Chiropractic care X-Rays must be clinically justifiable and have a causal link to the work-related injury or condition.
X-Rays can only be performed independently (in-clinic) by licensed chiropractors with approved X-ray machines and equipment.
Treatment Program Reviews
In cases where there is no positive response to chiropractic treatment, or if there is a need for further treatment after 6 weeks, a comprehensive review of the current treatment plan may be necessary. This review can include a referral to other allied healthcare providers or a change in treatment modality.
Coverage for the cost of reassessment or treatment program review is subject to approval from the insurer.
Supplementary Devices
The provision of treatment aid devices, such as braces or lumbar supports are covered by WorkCover, up to a maximum total of $249. Costs for supplementary treatment devices will require prior approval from the insurer.
Reports and Communication
A WorkCover claim will cover the cost of progress reports and time spent by your chiropractor communicating with your doctor or insurer.
What Chiropractic Conditions Are Covered by Workcover?
WorkCover claims apply to a wide range of spinal or musculoskeletal conditions that can be treated with chiropractic care. The main factor affecting eligibility is that the injury or condition must have been sustained or exacerbated due to work activity.
- Back Pain
- Disc Herniation / Disc Bulge
- Sciatica (Spinal nerve compression)
- Whiplash
- Spondylosis (Spinal osteoarthritis)
- Postural Issues
- Sacroiliac Joint (SIJ) Dysfunction
- Cervicogenic Headaches
- Scoliosis
- Temporomandibular Disorder (TMD)
- Carpal Tunnel Syndrome
Are There Out-of-Pocket Costs for WorkCover-Approved Chiro Treatment?
If your WorkCover claim has been approved, you will generally not need to pay any gap fees for chiropractic care. Your chiropractor must inform you beforehand if there are any out-of-pocket expenses for receiving certain services.
How To Submit A WorkCover Claim for Chiropractic Services
You are eligible to submit a WorkCover claim if you are an employed worker, whether in full-time, part-time, casual, or fixed-term capacity. Individuals under an apprenticeship or training program can also submit a claim. WorkCover eligibility for contractors, subcontractors, and volunteers is generally limited.
When you have sustained an injury at work or suspect that you need treatment for a condition, the first thing to do is to see your doctor (GP). During your consultation, request a Work Capacity Certificate from the doctor - this document is needed to submit a WorkCover claim.
When you have a Work Capacity Certificate that outlines your diagnosis, treatment plan and the capacity at which you can work, lodge the claim online at WorkSafe QLD. You will be given a claim number to pass on to the chiropractor during your consult.
Before you make a booking, ensure the chiropractor is registered with the Australian Health Practitioner Regulation Agency (AHPRA). WorkCover only compensates treatment undertaken by an AHPRA-registered chiropractor.
You can begin chiropractic care as soon as you have your claim number – the initial consultation and up to 5 subsequent treatment sessions are approved in advance with the insurer. Your chiropractor will manage the WorkCover claims on your behalf and bill the fees directly to your insurer.
WorkSafe Queensland has a 6-month time limit for submitting a WorkCover claim, starting from the date of the injury or the date of assessment during a doctor’s appointment (whichever is earlier).
Spinal Works Chiropractic is an AHPRA-registered and WorkCover-approved chiropractor in North Queensland. Our chiropractors apply the Gonstead Method and evidence-based treatments to help individuals recover from work injuries. Start your journey towards pain-free living today - get in touch with our chiropractic clinics in Townsville and Cairns to book a consultation.
Contact Us or Book Online
Contact us for more information or book an appointment online. Your path to pain-free living starts with Spinal Works Townsville and Cairns!